This microbe-filled pill could track inflammation in the gut
A blueberry-size pill that you swallow could let doctors measure signs of inflammatory bowel disease in the gut, helping spot it earlier and measure its progression in real time.
Nearly 70,000 people a year in the US are diagnosed with IBD, a class of conditions that includes Crohn’s and ulcerative colitis. Symptoms of this autoimmune disorder include fatigue, stomachache, rectal bleeding, and diarrhea. If left untreated, it can lead to colon cancer. Since its symptoms are shared by other diseases and can wax and wane, IBD is often diagnosed late, making it harder to treat.
“The gut is like a black box—very hard to access,” says Maria Inda, a synthetic biologist at MIT and co-leader on the team that created the pill. “The only way we have now is colonoscopy. That’s invasive, can’t be repeated at short intervals, and disrupts the gut microbiome.” Other tests depend on proxies of gut function like stool health, so they don’t give a real-time picture.
Inda and her colleagues created a pill containing E. coli bacteria that have been genetically engineered to detect nitric oxide, hydrogen peroxide, and other molecules that are produced in excess in the guts of people with IBD. A gene cluster was added to the bacteria that causes them to emit light when they are exposed to these inflammatory molecules. The pill also contains photodiodes, which can detect this light, and a radio chip that can transmit the signal outside the body. The team reported its initial findings in Nature earlier this year.
The team’s biggest challenge was finding a way to fit all this gear into an object small enough to be swallowed and not damage the stomach. “The goal was a functional device with enough signal but small enough to be safe for humans,” says Miguel Jimenez, a chemist at MIT who was Inda’s partner in developing this device. “Obviously the ideal would be microscopic size, but there are physical limits to the size of battery and diodes.”
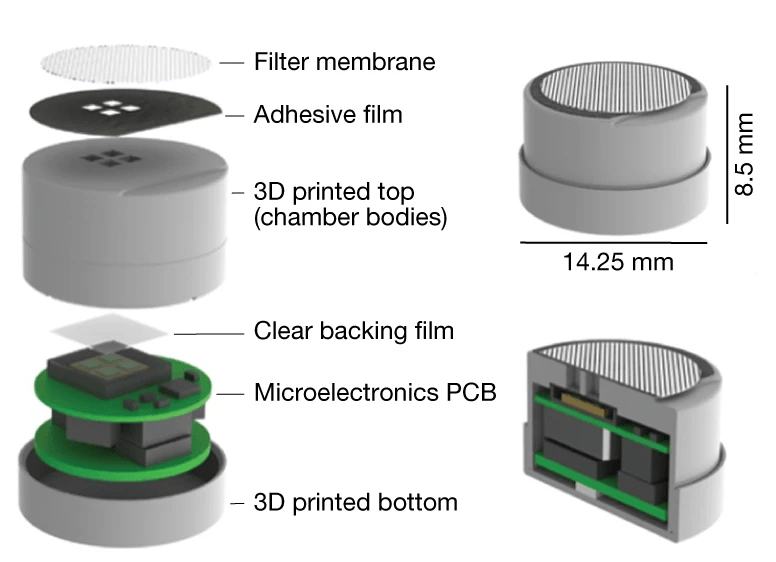
The team achieved the miniaturization by working out the minimum number of bacteria needed to emit a useful signal and making the electronics needed to detect, process, and transmit that signal as low-powered as possible. The next step was integrating the bacterial sensors with the electronics and fitting the whole setup inside a small package. This task was made trickier by the fact that the bacteria had to be maintained in a wet environment and the electronics had to be kept dry, which they accomplished by placing them on either side of a laser-cut adhesive film that was transparent to visible light. The whole system was then packaged into a 3D-printed casing, creating a bioelectronic pill with a volume of less than 1.4 cubic centimeters.
To test the pill’s efficacy, the researchers anesthetized pigs, surgically inserted the device into their intestines, and then closed them up. (“You can’t train them to swallow. If you were to just feed the device, they would chew it up,” says Jimenez.) The team found that the device was capable of picking up IBD biomarkers and sending a signal outside the pigs’ bodies. Inda adds that the pill now has to be validated in humans to demonstrate that the sensors are able to detect the biomarkers in the concentrations that would be indicative of disease.
Alessio Fasano, a gastroenterologist at Massachusetts General Hospital in Boston, says the bioelectronic pill is “futuristic.” His team is developing a “pill-cam,” a video capsule that can be swallowed to take pictures throughout the intestine and monitor visible areas of inflammation.
He says that having a noninvasive method to monitor changes in inflammation very early would be extremely useful. Catching patients’ frequent inflammatory flare-ups before the onset of symptoms could enable earlier intervention.
“This is a very innovative contribution in an area of dear clinical need,” he says.
